They have young patients to comfort, parents to reassure and, of course, incredibly delicate brain operations to perform. Amy Corderoy observes how a crack paediatric surgical team goes about its work as Brooke Mackenzie, 7, who has travelled from her home just outside Bathurst, undergoes brain surgery in Sydney.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The little girl whimpers as her mind struggles to free itself from the hold of the anaesthetic. Her scalp is raw, overlaid by large, dark stitches.
''It's a nervous time, waiting for them to wake up,'' paediatric brain surgeon Brian Owler says in an uncharacteristic moment of vulnerability.
''How many fingers am I holding up, Brooke?'' he asks in a soothing voice, only to hear her whimper again. ''You'll be OK … How many fingers am I holding up?''
No answer.
Only two months ago, seven-year-old Brooke Mackenzie, whose home is just outside Bathurst, was a little girl with a bad headache.
''They told me the next day it was maybe a migraine,'' says her mother, Linda Mackenzie.
Scans revealed an ominous spot, right in the centre of her brain.
No one knows for sure what is going on in Brooke's brain. Surgeons at the Children's Hospital at Westmead operate on about 50 new brain tumours every year and, of those, Owler estimates there are only about five in which the problem is unclear.
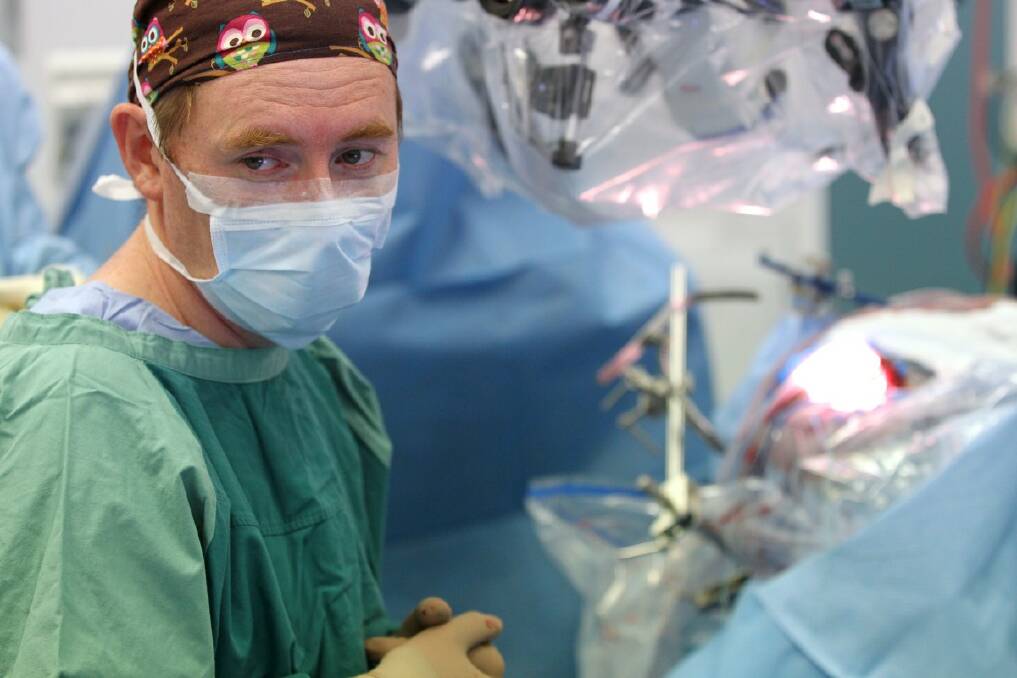
''You usually know what the problem is the moment a patient walks in the door,'' says Owler, the high-profile president of the Australian Medical Association's NSW branch.
The nervous wait for Brooke to wake up comes at the end of a typically long day for the highly specialised team at the hospital.
This theatre alone hosts about 1600 operations a year. Each is the eye of the storm for a family facing the kind of fears all hope to avoid.
The day begins just before 8am in a busy waiting room that is full of tired children and anxious parents. Owler talks to Lucinda Crowe, a 14-year-old with a ''Chiari malformation''. Her cerebellum is growing into her brain stem and pushing fluid into her spine, which is causing scoliosis.
Lucinda, who has Down syndrome, is scared and hungry, having had to refrain from eating before the surgery.
''She's been very brave,'' her mother, Jacqui White, says as she prepares to carry Lucinda into a room adjoining the operating theatre.
There, she is met by a nurse and two doctors, who will administer the complex anaesthetic that must be given to a child before operating on his or her brain.
Jacqui cradles Lucinda in her arms, gently stroking her back, as anaesthetist David Kinchington explains that he is going to give her some gas.
''What's your favourite colour?'' he asks Lucinda. This flows into a question about drawing and if the smell from the mask reminds her of her favourite coloured textas.
And she's out. The team place her on her stomach, her head held in place off the end of the bed by a metal stand.
The cut itself is surprisingly small. A couple of inches in the back, where the team's members will place a small patch to create more room.
As they continue to work, Aretha Franklin belts out Think from Kinchington's iPod.
They insert a tiny plastic ''tent'' into her skull, held up by small metal pieces, and, after stitching her back up, she is even able to lie on the wound.
Owler and surgical registrar Chris Daly next review Brooke's scans. This will be a bigger job.
Her headaches have eased and the lesion on her brain seems to have become more difficult to see on the scans.
We head back to the waiting room to sit with Linda and Brooke, while Owler consults with the radiology team about the scans.
Linda is scared. ''I'm just waiting for them to say everything went well and it's out,'' she says.
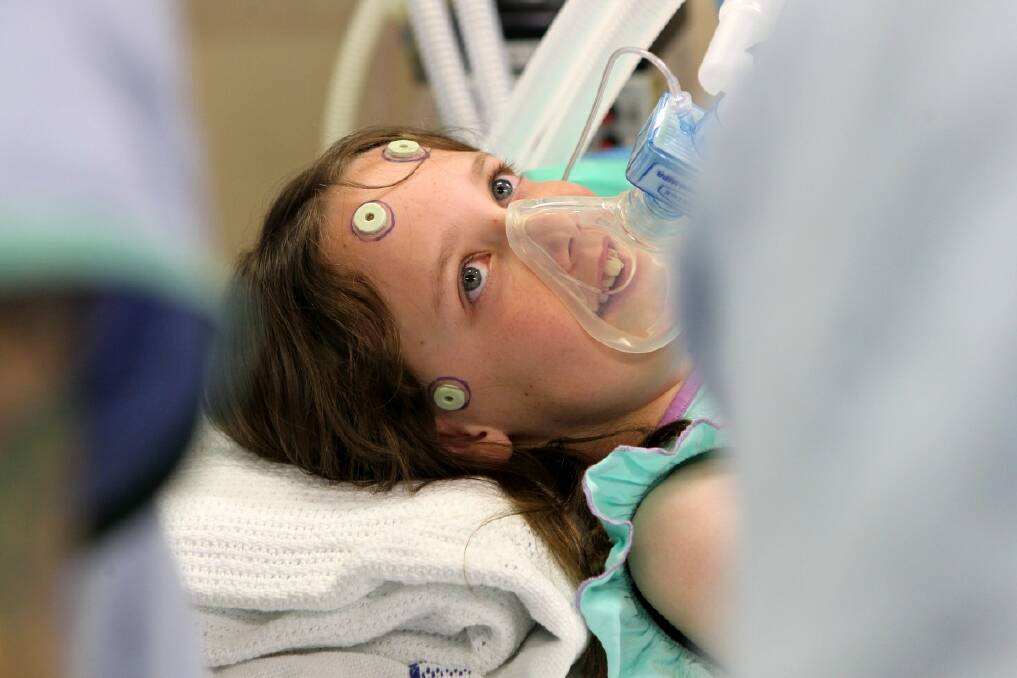
Brooke, on the other hand, seems happy, although she has strange dots stuck all over her head, which will be used to guide the surgeons during the procedure.
''She's got 'go', this one,'' her aunt, Joanne Harper, says later.
''Every time she's seen a billboard for weeks she's been shouting, 'There's my doctor! There's my doctor!''' Linda says, referring to Owler's high-profile role in the ''Don't Rush'' road safety advertising campaign.
The doctors and nurses adapt their demeanour to match Brooke.
''This medicine makes you go 'wooooohh','' Kinchington says as he begins to put her under. ''It makes our jokes better.''
As Linda leaves the room, her eyes fill with tears.
Daly begins to shave Brooke's head. ''Not too much hair, you'll be in trouble,'' Owler says.
It is these little things that can cause the most distress for patients, he says. Never privy to the incredibly delicate and invasive surgery, it is the bumps and strange sights on which they focus.
As the opening verse of A Little Ray of Sunshine wafts across the room, Owler makes the first clean, smooth cut straight across the right side of Brooke's scalp.
The wound is shocking. To prevent visible scarring across Brooke's face, a larger incision must be made further back in her hairline and her scalp pushed back out of the way.
Then a circular piece of her skull, about 10 centimetres in diameter, is carefully cut. Her brain sits, exposed. Pulsing with every beat of her heart.
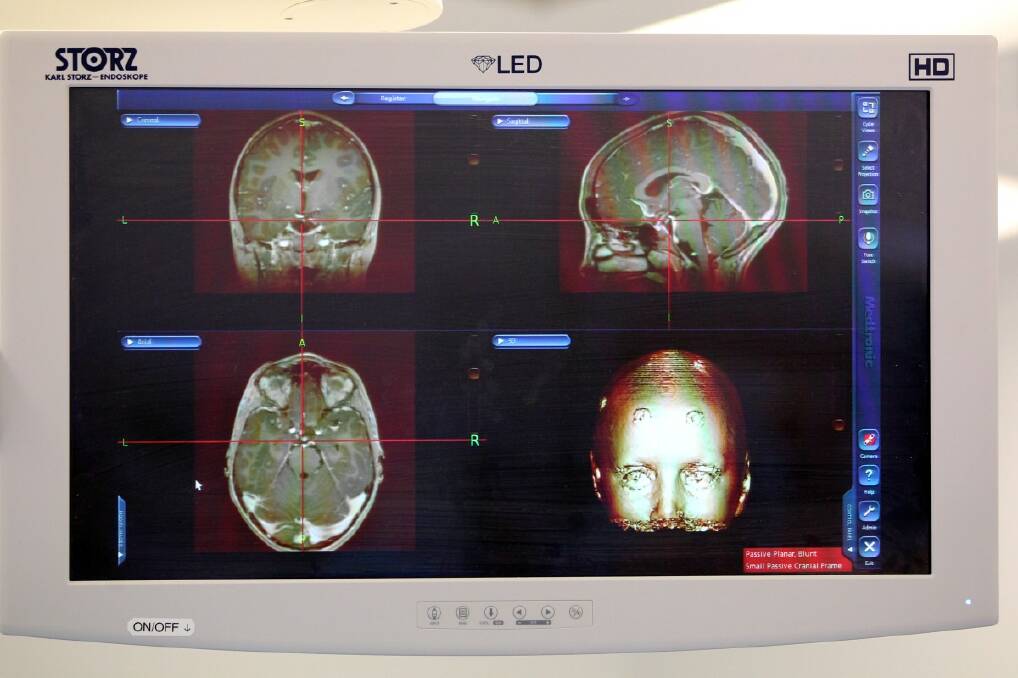
''We want to traumatise the brain as little as possible, so we've got to sneak in under the frontal lobe,'' Owler says. Brooke's head is mapped onto a scan and those dots, called fiducials, are helping Owler pinpoint his actions against it.
This type of machine has been around since the turn of the century and has drastically changed surgery, Owler says.
If the money were available, he would have an intraoperative MRI, which would allow him to do a live scan during an operation.
Deeper in he goes, until he reaches the basilar artery, which supplies blood to the brain stem, the powerhouse through which important messages from the body travel.
Then the optic nerve and the olfactory tract. The slightest wrong move could damage her vision or sense of smell permanently.
But something looks wrong. The clean, almost translucent white of the membranes that thread through the brain are discoloured.
Owler sees the tumour, protruding from the optic nerve. It cannot be completely removed without destroying Brooke's sight.
He carefully cuts the rest away, as close as he can to the optic nerve, taking small samples that are immediately sent to the pathology lab.
We wait. The music from an MP3 player is the only sound in the room.
Suddenly, the phone hanging on the operating theatre wall trills. The report: it's a low-grade glial tumour. It is not aggressive, it will not kill her. But the remaining cells could grow back and damage her sight.
''I'm not sure if it's bad news or if it's good news,'' Owler says.
''It could be a lot worse,'' nurse Liz Buchannan says. They have seen a lot of bad news in this room.
There is nothing left to do but put Brooke back together again. One of the drugs she has been given has dehydrated her brain and it sits, still pulsing but now smaller inside its skull. Owler and Daly give it a squirt of saline-like solution on to help it to rehydrate.
Daly takes the piece of her skull removed earlier and attaches little silver plates that will be used to screw it back in place. The join between them will be smoothed over by putty.
''The scalp is very vascular,'' Owler says as the blue clips that have been holding it in place are removed. Suddenly, there is blood everywhere.
Daly ignores it, stitching with a quick hand. Some surgeons can panic but the best thing to do is to just keep stitching through it, Owler says.
After the operation, he has made up his mind: of all the possibilities, this is good news.
''It went quite well, we got most of it out,'' he says.
They remove the layers of protective sheeting covering Brooke's body and head, preparing to wake her up. Daly carefully washes her hair.
The room is quiet again and then we hear her whimper. ''How many fingers am I holding up, Brooke?'' Owler asks.
Her eyes are dazed, she is confused.
''It's OK Brooke, you'll be OK. How many fingers am I holding up?'' No answer. And then, she slowly raises her little hand up to his, reaching out to touch him.
She can see. ''Good girl, Brooke, you're OK,'' he says, stroking her head.
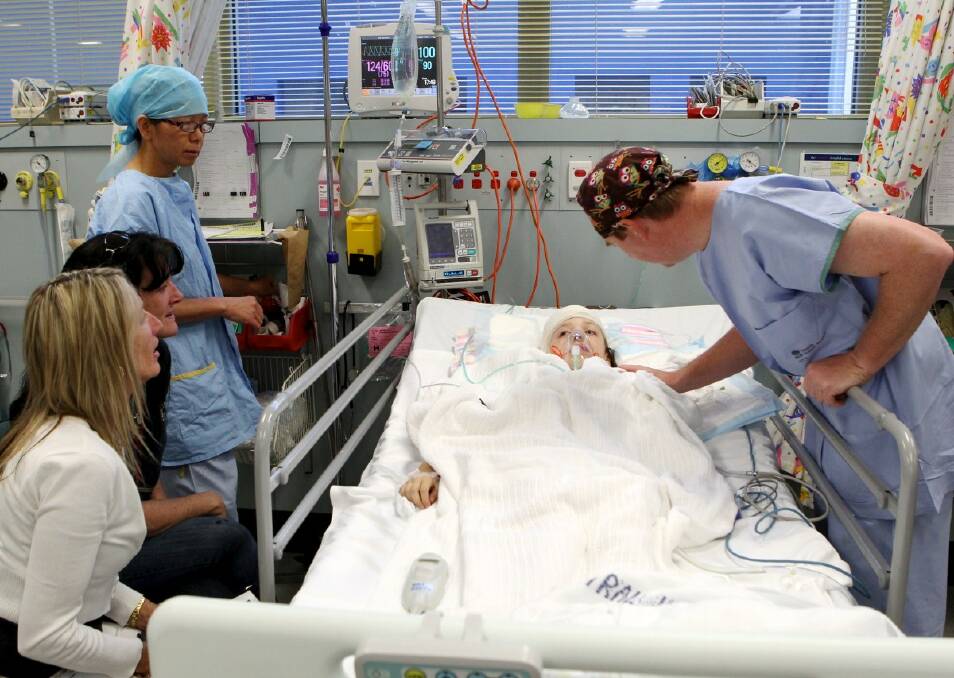
When Linda finally sees her daughter, about an hour later, the shock hits her like a physical blow.
''She doesn't look all right,'' she says, tears streaming down her face. She stares, blank-faced and crying, at her little girl. Brooke is barely awake, drifting in and out, painkillers flooding through her system.
''I just haven't seen her like that, ever,'' she says.
Owler says even adults undergoing this kind of surgery sometimes have trouble coping.
''I can't imagine, not only for the child but for the family, how they cope with going through it,'' he says.
Linda will stay in the ward the coming night to be with Brooke, before moving back to a hotel while she continues her treatment. The family home, just outside Bathurst, is a long way away.
After her initial distress, just a week later she is ecstatic.
It is possible Brooke will have some vision problems and she might need low-level chemotherapy to treat the remaining tumour cells.
''But she's feeling really really good,'' Linda says. ''She's doing craft and she's got her appetite back. She's even liking all these different, new foods and she says she can smell things better. They say that happens sometimes after brain surgery.''
Her wound does not stand out.
''Dr Owler said she had lovely hair and there's hardly any hair gone,'' she says. ''I couldn't have asked for any better.''